
Randy Ballard enters his 13th season as an athletic trainer for the volleyball, cross country and track and field teams. A 1999 graduate of Kansas State University, Ballard earned his master’s degree in kinesiology from the University of Texas in 2001. The Concordia, Kan., native is no stranger to working with world-class athletes. Ballard has worked as an athletic trainer several times for the USA Track & Field teams. Most recently, he served as an athletic trainer for USA Track and Field at the 2008 Olympic Games in Beijing, China. The previous year, Ballard was an athletic trainer for the 2007 U.S. Track & Field World Championships team in Osaka, Japan. He also served as the Head Athletic Trainer at the 2006 Cross Country World Championships in Fukuoka, Japan. He has also served as therapist for numerous Olympians and world champions including Perdita Felicien, Bershawn Jackson, and Lauren Williams.
Randy has a great interest and expertise in manual therapies and the rehabilitation aspects of the athletic training world. Having learned from numerous well-renowned therapists, Ballard brings a well-rounded skill set to the athletic training room. Along with being integral in the therapy and rehabilitation aspects of sports medicine, Ballard helped develop the physical competency testing that the volleyball team uses to help assess and develop their training programming. Randy has also presented at several professional and coaching conferences on therapy, testing and rehabilitation topics.
Prior to Illinois, Ballard spent three seasons as a student athletic trainer for the Kansas State athletic program before moving to Texas. In Austin, Ballard worked primarily with the Longhorn football and men’s track and field programs. (Source University of Illinois)
Athlete Screening
Freelap USA — You screen athletes with something called the Physical Competence Assessment (PCA), something not commonly known in the US. Being highly respected by track coaches and well known for your work with runners, what can you share about the differences between the Functional Movement Screen (FMS) and PCA that make you an adopter?
Ballard — For me the three biggest things about the PCA that I prefer are as follows. One is that the PCA lends itself to building a testing system that fits your situation, your athletes and your needs, not banking on the seven same tests giving you all the answers you need. Based on Key Performance Indicators (KPI’s), what I like to call key postural positions, injury histories, common issues, etc, it allows the coach/therapist team to build an assessment that fits their needs. Secondly, the PCA contains specific tasks that I feel the FMS is lacking which are essential in evaluating athletes. These include one leg tasks, such as one leg squat that make more sense to me for athletes and runners, as well as landing tasks which for me help paint a better picture of the underlying issues in the athlete. Finally, if you’re going to build an assessment system you need to have a plan of what you’re going to do with the data and who is going to be responsible for what, i.e. testing is step one, you need step two and three figured out before you start. For me, step 2 and 3, often involve collaborating with the coach, S&C, and the athlete. In my experience, it has been easier to drive this collaboration by utilizing movement tasks that are more familiar and foundational for sport coaches than the 7 tests the FMS prescribes.
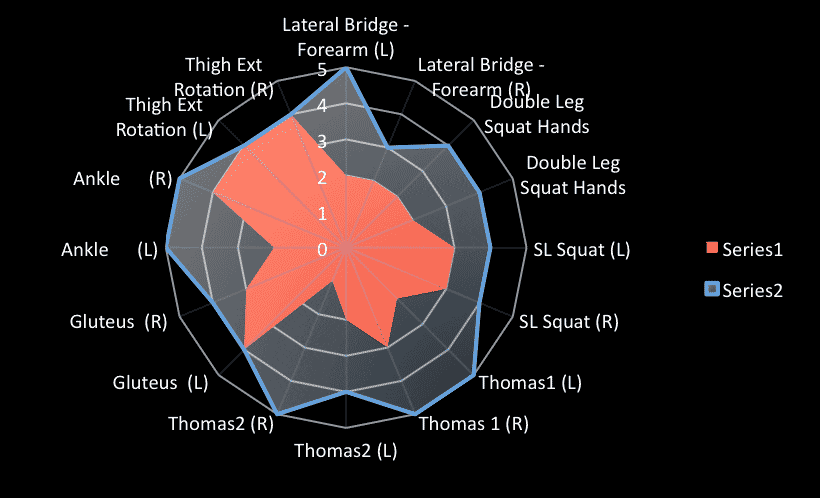
Plot 1: Radar plots or spider charts are a good way to summarize all of the data during the Physical Competence Assessment (PCA) screening to visualize how the interventions are shaping up.
Carl’s Take — A key take home message is to do what you need to do to get the job done and be agnostic to trends or “systems” out there. Feel free to adjust whatever resources you need to do to make things work. I think the evolution to screening speed and power athletes is to reverse engineer injuries that are common to the sport, look at the causes of why they happen, and use testing or evaluation techniques to look for risk factors. Risk factors may be very static (anatomical) or more variable (strength or muscle tone) so interventions that are effective are extremely important. I am agnostic to screening but as technology increases we will see conventional screening approaches be combined with motion capture, wireless EMG, pressure mapping, and even physiological data to see how fatigue factors into the screening process. Also, the PCA converted into more appropriate scoring such as degrees makes for a very precise way to use Radar charts. I don’t use Radar charts often, but if you are collecting data for years they create patterns or shapes that are very useful for showing how the season factors in. So long as the testing is organized consistently, you will find classifications of injury patterns based on both training data and medical testing.
Evaluating Manual Therapists for Sports Medicine
Freelap USA — Manual therapy is essential for many injuries and athletes tend to be lured in by high profile therapists touting all these systems with three letters next to them. Without spending too much time, how should a coach and athlete pursue manual therapy to improve tissues and joint function? What are some general qualities that can make the sprint community a more educated shopper?
Ballard — I think there are some tale-tale signs of whether a therapist gets it or not and whether they are in it for the right reasons. Often, the therapist that is seeking out the athlete or coach has alternative motives and isn’t going to be a great fit. To have better outcomes, a good therapists is going to have more than one tool in their toolbox, ideally multiple tools (and I’m not just talking about soft-tissue mobilization tools.) I’m always hesitant when I talk with a fellow therapist and they focus on one system that they think fixes all the problems, very rarely is this the case in dealing with significant soft-tissue issues, let alone maintaining optimal tissue function during heavy training. I think the therapist needs to be a role player and understand that from the beginning. To be a great role player, communication and collaboration are key. Can they speak the same language and see the same things, or at least understand the things the coach is seeing and the athlete is explaining. The final thing is that the therapist must understand the event, demands, and how their piece of the puzzle fits into the training and planning. Therapy is another stimulus that is being added into the global system. This stimulus must be well thought out and dosed appropriately, in relation to frequency, timing, and training. If your therapist doesn’t understand this, you’re setting up your athlete for a less than ideal situation, therapy being counterproductive, and/or more problems than fixes.
Carl’s Take — One of the most important choices outside of coaching is to get the right therapist. A good therapist is one that actually does manual work, not just suggesting exercises. Manual therapy is expensive because the best are usually working with elites but some great therapists exist that may not have impressive resumes or testimonials. I know several great therapists that are constantly working with elites because they referred to by other athletes and coaches. Remember athletes vote by their feet, meaning are they willing to travel to work with the therapist and do they come back over and over. Sports massage is one of the best values and don’t get caught by therapists who are gurus, since many are not willing to put the time and hard work with hands on treatment. Massage is hard work and those that avoid the hands on approach are usually charging for fluff. The best way to test is allowing them to go hard and reduce elbows and instrumentation, since scraping usually creates too much trauma.
Applied Athlete Monitoring: A Medical Perspective
Freelap USA — When dealing with common illness and injuries, monitoring is a process of both objective and subjective analysis. Could you share how blood testing, subjective indicators, and careful training volumes be integrated in a college setting? You have years of data and have worked with an array of track athletes. Any suggestions?
Ballard — I think initially the most important piece of this is reminding yourself your dealing with college kids. You must realize that while your data is going to give you feedback on things, you must have plans of how your are going to use it, and it most cases, this involves education and impacting team cultures. We have to educate coaches and teams on the importance of this piece if there is going to be compliance and follow-thru. We then have to educate and spark lifestyle changes and team culture changes. I suggest starting simple, do some basic panels at a set frequency such as Complete Blood Count (CBC), ferritin, and Vitamin D, four times a year. Based on results, plan how you can use this information to educate your athletes and coaches, and then figure out the next layer to add on, once you’ve established buy-in, compliance and a culture where it is valued. What’s the point of continuing to build a testing system if kids aren’t willing to be adults and listen, learn, and adapt. Honestly, it doesn’t matter how great your testing system is, if you can’t be an educator, salesman, and team culture architect, a lot of this is just gathering numbers for nothing. Finally, realize while these are often specific markers, they are painting a global picture of what is going on with that athlete and within that team. For example, if a sophomore distance runner’s ferritin drops 20 points between mid-August and mid-October is it just because the coach upped their mileage twenty percent from last year? Or is it because it was the hottest fall in years, it’s the first time the young person has lived outside of the dorms or mom’s house and has no idea how to grocery shop or cook, or is it because they are living with three fellow teammates who are as clueless and immature and aren’t holding each other accountable?
Plot 2: Heart Rate Variability (HRV) is an effective tool to monitor trends in autonomic status of the body, and simple solutions that done longitudinally are the best options. The above plot shows the use of specific bandlines to help show risk zones and potential peaking periods.
Carl’s Take — Readers should note that a combination of HRV, subjective indicators, and blood monitoring are used to connect the dots. The compliance and resourcefulness of what Randy does is amazing and is something you can’t build overnight without putting in the time on educational support after testing. I am a huge fan of subjective indicators that lead to more and better questions and feel that blood analysis quarterly really can reduce complicated problems from surfacing. For example I spoke openly about how complicated ferritin status can be since several nutritious foods can compete for absorption and even drinking coffee at the wrong time can be a death sentence for some athlete who are in midseason and trying to climb out of a hole. Combined with genetic testing and Near Infrared Spectroscopy (NIRS), hemoglobin fluctuations from blood plasma changes will help keep athletes from fatigue. I have been trying to create an enterprise solution for Rapid Introspective Video Analysis Logs (RIVAL) by letting athletes do a quick, 30 seconds, Instagram videos privately and look for emotional readings to help save time. With facial coding software we can get a lot of data outside word analysis of athletes, and this is far better than the emoticons we are seeing with some athlete management software showcased at conferences.
Treating “Shin Splints” or Tibial Stress Syndromes
Freelap USA — Shin splints are common in running events ranging from the 60 m dash to marathon. What are your best solutions here with an injury pattern that is frankly accepted too easily? Any comprehensive solutions in working with this overuse injury? Any resources here or ideas?
Ballard — I think realizing just because its common, doesn’t mean it is a simple fix. It’s very multifaceted and takes a multifaceted approach. One of the first things I look at are mechanics. Being around Gary for all of those years, I learned tremendously about the need for stiffness thru the foot and ankle and the need for a reactive foot strike. I like to start there and then work up. Obviously the research highlights for the importance of lumbo/pelvic/hip strength and integrity and we need to feel that out. The PCA can be a useful tool for this but it could be as basic as manual muscle testing. Another tool I use, while low tech is to rub the foot with sidewalk chalk and have the athlete walk on the dark floor of my training room looking for abnormal pressure patterns or if they are optimally loading thru the great toe or other issues that can set up the biomechanical overload thru the medial shin. Therapy-wise, I often look to the musculotendon juncture of gastric/soleus/achilles, not just at the medial tissues. This tissue is often not optimal and needs addressed with more than a foam roller. The tissues of the plantar aspects of the foot also need to be pliable and mobile and should be addressed if need be. Finally, on the rehab side of things I try to program to address the stiffness thru the foot/ankle, eccentric work thru the lower extremity, and working to get everything functioning together for optimal foot-strike and lower ground contact time. As you can tell, I’m often a chili pot of ideas and approaches. In this case, its equal helpings of Gary Winckler, Boo Schexnayder, Dr. Andy Franklyn-Miller, Dr. Bruce Williams, and some research.
Carl’s Take — Foot strike is essential to a healthy lower limb and perhaps all the way up to the spine. The body can only tolerate so much and when juggling fatigue, the natural buffer zone of risk gap will be different based on anatomy, training program, surfaces and footwear, and manual support. Very little can be done to develop the intrinsic muscles of the foot beyond just keeping things engaged, and barefoot training has pros and cons like any other modality. The timeless adage of everything in moderation is a good fit here with barefoot or minimalism training. Most of the interventions are managing the training program and evaluating foot function with very comprehensive evaluation. Orthotics are static interventions are extremely individualized and I never suggest a design without pressure mapping and doing sEMG. 3-D Motion capture is valuable, but what is important is that the relationships between all of the variables are what is truly needed for conformation. Good data, is a summary of the findings that rule out everything.
Combining Sport Psychology and Sports Medicine
Freelap USA — The psychology of injury tends to be left behind outside of some contemporary discussions on pain. Any good stories you can share of dealing with the recovery process from a psychological standpoint? I can see with the popularity of pain science and the emotional scars of getting hurt makes things far more complicated than stretching and exercises! Anything you can share to educate coaches and athletes?
Ballard — For me its starts before the injury. I work hard to build a rapport with my athletes that establishes a high level confidence in my abilities that is hard to waiver. I think the athlete’s confidence in their therapist/ATC/rehab team, is essential to overcome any psych rooted issues that follow injuries. This rapport not only lends itself to this confidence but also to a relationship that allows me to identify and work thru these psych/emotional issues during the early stages of rehab. Just as the tissue needs to go thru the healing cycle stages, we need to have the psyche and emotional aspects scarred in and stressed before pushing the rehab intensity and advancement. Finally, getting the athlete out of the training room and back to their territory is crucial. I try to do as much stuff at the track and weight room and out of the training room as we can to help the athlete to feel at home and relaxed. One related story that stands out is often times, we see these athletes, especially the sprinters, being hyper focused on the area of the injury. In these instances, I’ve found tasks such as jump rope running or others that shifts the athletes focus to something else, besides the tissue, to be great breakout rehab sessions. This allows them to put in work, then allows for the follow up discussion between coach, athlete, and therapist on their return and optimal mental state and arousal.
Carl’s Take — Rehabilitation from injury with athletes is a different dynamic than conventional PT and while a lot of similarities exist, the difference is the return to play strategy that reduces risk of re-injury. Positive energy is what I feel separates great therapists from the best, since the information or expertise may not be that much different. Athletes should have a rewarding experience that gives them confidence and the right balance of patient education that doesn’t make them overloaded with fear and doubt. Guarding the body from the wrong information delivery is what I am seeing to be a common problem now as many medical professionals, wanting to prove themselves, are creating a backfiring event.
Please share this article so others may benefit.
[mashshare]

