
My Story
I’m lying on my side with an oxygen mask over my mouth. The anaesthetist is sitting next to me. It seems to take an age for me to understand what he is saying; “Can you feel that? Does it hurt?” In my head, I slowly register his words through the fog of sedation. It does hurt; it hurts a lot. And it would hurt – after using a hammer to insert a metal tube into my spine, my surgeon is now using a saw to cut out bits of my disc. I’m kept awake so that I can move my leg if required, which is an important step to make sure I’m not suffering any permanent nerve damage. Although sedated, I can feel pain. Fortunately, my anaesthetist can turn up the sedation and put me to sleep, putting a temporary end to it all. After three hours of surgery (which was supposed to only last 45 minutes), I am wheeled into the recovery room to wake up fully. This is where the most painful experience of the whole operation occurs. All the deep tissue that lies around the spine, which has been in spasm for three months to protect the area of instability, suddenly realises it can relax a bit. All the toxins and waste products that have been building up in the tissue are released, and an intense feeling of pain hits me in my lower abdomen, which lasts for about 15 minutes, until the pain killers administered by the nurse kick in.
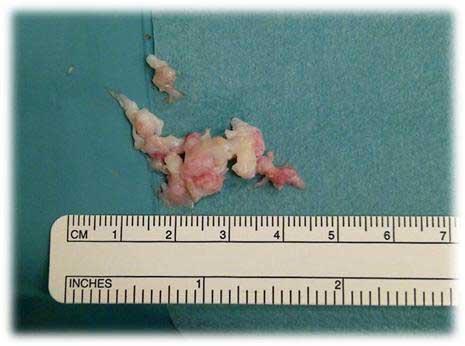
Figure 1: Disc that was removed during surgery.
So, how did I get to this point? I suffered my first real back injury when I was 18. Although I didn’t have an MRI scan on that occasion, judging by the symptoms I experienced, I was probably suffering from a disc issue. Then, when I was 20, it came back again. My back would seize up from time to time, making any activity difficult for a few days. It had a nasty habit of doing so in warm-ups for races, which made running difficult. This time, I did have an MRI scan, which showed dehydrated discs and a few protrusions in my lumbar spine. A plan was devised to work our way round this problem, and I managed well, suffering no real back symptoms after that year for the following three competitive seasons.
Then, in 2011, I was in the gym doing deadlifts. I’d love to say I was lifting a heavy weight, but the truth is I wasn’t – it was only about 60% of my rep maximum. About halfway through the set, I lifted the weight from the floor, and as I did, I remembered thinking that my back position wasn’t quite right. As soon as I thought this, I felt a weird shift in my back, like something moving backwards, followed by a shot of pain at that specific site, which then transformed into a very global, very severe pain. Every single muscle, from my knees to my neck, had spasmed. The spasm on my right side was so great that it pulled my pelvis towards that side, which made walking pretty hard. An MRI scan showed a pretty severe disc bulge in one of my troublesome lumbar discs. I rehabilitated for the next 12 weeks, got back into some decent running, and managed to run 10.19 that season.
Off the back of this 2011 season, I was all ready to go to the 2012 Olympics, which were taking place in my home country. I had been looking forward to this for ages, had moved to a place and a training group I thought could enable me to do this, and had just had a reasonably successful season despite missing a lot of training due to my back. I can’t remember the exact day I started to feel pain in my right hip, but it was around the start of November. I had another MRI, which showed that one of my discs had further degenerated, and would probably require surgery in about five years. As November turned into December, my symptoms were slowly getting worse; I’d wake up in the night and not be able to feel my right foot. I wouldn’t be able to lift my right leg high enough when running—all classic signs of reasonably severe disc dysfunction. But, because I wanted more than anything to qualify for the Olympics, I pushed it to the back of my mind. Another MRI in December showed that I would probably need surgery after the Olympics; that was fine by me as long as I could get there. At the end of December, I had an epidural and some injections in my back to settle down the symptoms and traveled to South Africa for a warm weather training camp. On the fifth day there, I woke up one morning, unable to move. There was no acute incident; I only went to sleep one night, and I woke up a wreck. I knew then that this was very, very bad. I didn’t train for the rest of the camp; I flew home and saw the surgeon, who recommended surgery. My MRI now showed a herniated disc severely impinging on my sciatic nerve. My surgery was set up for two months later. Living through those two months was tough; because my sciatic nerve was affected to such a degree, I was comfortable only in two positions, exactly straight (standing or lying) and exactly on my left side. Every other position caused excruciating pain and pressure in my leg. If I wanted to sneeze (when I had a cold), I used to have to stand in a doorway, brace my body and head against the door frame, and sneeze there to prevent my head from jerking forward, which was agony.
Fortunately, my surgery went well, and I ended up with about 50% of my L3-4 disc getting removed. I slowly rehabilitated myself, switched to bobsleigh, and got selected for the Winter Olympics. Sadly, once I was there, my back injury flared up again, and I was forced to withdraw and retire.
Why do we get injured?
If you are reading this and have taken part in sports at any level, you will have suffered a sporting injury. My back injury was on the severe end of the spectrum, but injury is something we all have to deal with. There are two types of injury: chronic and acute. An acute injury is a sudden onset, and the inciting event is identified by the application of some external force (Meeuwisse 1994). A chronic injury is an overuse injury, where repetitive micro trauma eventually causes an injury. But why do we get injured? Bahr and Krosshaug (2005) developed the “Comprehensive model for injury causation,” and, as the title suggests, it is very comprehensive! For an injury to happen, they state that there is an inciting event on a susceptible athlete. The more susceptible the athlete, or the more severe the inciting event, the greater the chance of injury.
Internal Risk Factors
Bahr and Krosshaug identified the following internal risk factors that make an athlete predisposed to injury:
- Age (maturation, aging)
- Gender
- Body composition (weight, fat mass, anthropometrics, bone mineral density)
- Health (history of previous injury, joint instability)
- Physical Fitness (strength, power, resistance to fatigue, joint ROM)
- Anatomy
- Skill Level (technique, postural stability)
- Psychological factors (competitiveness, motivation, perception of risk).
How well athletes score in these regions depends on how susceptible they are to injury. Take gender, for example. Being a woman significantly increases your chances of suffering anterior cruciate ligament injury (Arendt and Dick, 1995), potentially due to increased femoral tilt.
Interestingly, recent research has shown that our genetics can increase our predisposition to certain injuries. For example, a specific variant of the COL5A1 gene is associated with chronic Achilles tendinopathy (September et al., 2009).
Take my back injury as an example. I was at a massive risk of injury at that point of my career. I was genetically predispositioned to suffer from a back injury due to a syndrome I have, which means I have enlarged transverse processes, reducing my flexion and extension range, which, in turn, puts more pressure on my discs. (I’ve also recently had a DNA test done, in which I scored off the chart for injury risk!) I had a lot of previous injury in this area, which is an additional risk factor. My previous injuries had probably affected my movement patterning, which meant I wasn’t strong enough in certain movements, placing my already at-risk back in further likelihood of injury.
Exposure to extrinsic factors
Once an athlete with a high injury predisposition is exposed to external risk factors, the chance for injury is further increased. The external risk factors include sports factors, such as rules, protective equipment, and the environment. Within track and field, examples include a high training volume on a hard running surface potentially increasing the risk of shin injuries in athletes, or training outside in cold temperatures potentially increasing the chance of a musculoskeletal injury.
Using bobsleigh as an example, the environment in which the sport takes part is usually cold (I recall competing in -27 degrees Celsius), which increases the chance of musculoskeletal injury. There is also the possibility of injury from crashing, either an impact injury against the bobsleigh or track, or an ice burn from being held against the ice whilst being upside-down, travelling at 80 miles per hour. To reduce the risk of injury, we wear helmets and burns vests and strengthen our exposed areas to be able to handle the impact better.
Inciting Event
When we have a susceptible athlete who then comes into contact with an inciting event, then we have an injury risk. An inciting event could be a game-based situation, such as contact with another player or object, or falling over. It could be down to a biomechanical issue, such as a player changing direction and injuring his or her knee. In the case of a chronic injury, the inciting event could occur over a long period, eventually causing injury.
The inciting event for the injury that caused me to retire was pulling the brakes in the back of a bobsleigh. Pulling the brakes is a loaded spinal extension exercise, going from a position of sustained maximal spinal flexion to extension whilst pulling a load. I was already a severely at-risk athlete, taking part in an activity that exposed to me significant external risk factors (early morning activity, cold weather, technical requirements of maintaining extreme spinal flexion), which meant the chance of an inciting event was high. Had it not happened at that particular time, on that particular day, I strongly believe it would have happened at some point close to that, due to the fact that both the intrinsic and extrinsic risk factors were so great.
Can we predict an injury?
Once we know why we get injured, it would be useful to know if we can predict the chances of us getting injured. There is some evidence that we can. Obviously, every single athlete is predisposed to injury in some way through the mix of intrinsic and extrinsic factors, but there are ways we can predict who is more likely to be injured. The first is through a screening process. Gray Cook developed the Functional Movement Screen (FMS), which assesses athlete’s competencies at a variety of movements. Athletes that score poorly on the test are thought to be at more risk of injury. The jury is still out on the usefulness of screens such as the FMS. Kiesel et al. (2007) used the FMS in pre-season training with a football team and found that those that scored poorly were more likely to report an injury over the playing season. Freckleton et al. (2014) tested single leg hip bridging in a group of Australian Rules Football players in their preseason. The players that showed one leg to be significantly weaker than the other were much more likely to injure the hamstring in the weaker leg over the course of the season. Although it is still early days, genetic testing might be useful to give a picture of injury risk. Collins and Raleigh (2009) found that there is a wide variety of genes potentially associated with musculoskeletal injury. The ability to test genetics and use movement screens is potentially a really useful way to create effective training programmes to lower the injury risk.
Periods of high intensity or high volume of training are also a potential point of injury. Hullin et al. (2014) found that large increases in workload in a group of elite cricket fast bowlers were a reliable indicator of increased injury risk.
Poor nutritional status is also a risk factor for injury. Athletes that are in energy deficit are more likely to be in a fatigued state (as their recovery is potentially compromised) and so are at an increased injury risk. Various micronutrients also play a role in injury, including calcium and magnesium in bone health. Low levels of vitamin D have been linked to a decrease in bone mineral density as well the loss of muscle strength (Cannell et al., 2009). Athletes are generally vitamin D deficient, and so this is an easily modifiable risk factor.
How do we reduce our chances of getting injured?

Figure 2: Boxers wearing gloves and protective headgear. WCAP boxers medal at U.S. National Championships – FMWRC by US Army
Is there anything we can do to prevent ourselves or our athletes from getting injured? In a recent meta-analysis on the effectiveness of injury prevention techniques, Lauersen et al. (2014) found that strength training is highly significant in reducing injuries. The mechanism for this is that the musculoskeletal system adapts to strength training, allowing the athlete to handle high loads more easily. Proprioceptive and co-ordination training were also shown to be helpful in reducing the injury risk. However, passive stretching pre-training or pre-competition does not show any protective effect. In my opinion, if a muscle is tight enough to restrict the range of motion at a joint, then this places you at an increased injury risk, and steps should be taken to address this. Chronic tightness in a muscle increases the chance of injury in that muscle through a variety of factors, and also potentially increases the global injury risk as it could cause other muscles to have to overwork.
Tips to Reduce Injury Risk
- Consider a regular physical screening to assess current movement competencies, and pick up on any imbalances or strength deficits that may contribute to injury.
- Ensure appropriate strength training is in place with adequate and sensible progressions for your age and maturation.
- Make sure that your body composition is at the correct level for your sport. Being too heavy can increase the stress and force going through your joints, muscles, and ligaments. Some adipose tissue may be useful in contact sports to protect against impact.
- Consider the sport specific demands of what you do, and ensure that your body can meet these demands. As a case in point, when I converted to bobsleigh, I had to ensure I could hold and maintain a large amount of spinal flexion in the back of the bobsleigh. To begin with, I couldn’t, but I designed a pre-habilitation programme to enable me to do this. Soccer players require greater conditioning of the ankles in order to handle cutting movements and also reduce the risk of ankle sprains in a tackle. An additional bobsleigh example of my own was the need to increase my neck strength so that if we ever crashed, I could use my head to lift my body off the ice, preventing ice burns. With regard to sprinting, the hamstrings have to be able to handle a large eccentric load throughout the sprint cycle, so they should be adequately conditioned to manage this task.
- Try to avoid large, sudden increases in training volume or intensity. If these can’t be avoided, then ensure that appropriate recovery techniques are used.
- Strive to meet the energy demands of your sport. Training and competing in a fatigued state increases the injury risk, so make sure you are conditioned enough to meet the demands.
- Ensure that you have an adequate range of motion in the correct joints and that all areas are working well. If one joint has a less-than-adequate range of motion, it increases the chance of injury in that area and the pressure on the surrounding joints.
- Fully recover from any previous injury. Keep rehabilitation going until there is no strength deficit in the muscle and normal motor patterning has returned.
- Make sure your nutritional status is good; you should get sufficient vitamins and minerals to ensure that your bones and immune system are healthy.
- Work on your posture and ability to hold this posture under fatigue. Being in the correct position at the correct time ensures optimal technique, which reduces injury risk. Being able to contract the right muscles at the right time is crucial to reduce injury risk. Let me illustrate this point: I currently suffer from right knee pain because my right gluteus medius has atrophied (due to nerve damage), so, under load, I can’t control my thigh as well as I used to in the past.
- Make sure you aid your recovery from training. Sufficient sleep is important!
- Improve your technique as much as possible. Poor technique is a risk factor for injury as it is usually less economical and can overload certain muscle groups.
Please share this article so others may benefit.
[mashshare]Further Reading
Becoming A Supple Leopard: The Ultimate Guide To Resolving Pain, Preventing Injury, and Optimizing Athletic Performance by Kelly Starrett
Ready To Run: Unlocking Your Potential To Run Naturally by Kelly Starrett and TJ Murphy
Athletic Body In Balance by Gray Cook
Movement – Functional Movement Systems: Screening, Assessment, Corrective Strategies by Gray Cook
References
Arendt, E., & Dick, R. (1995). Knee injury patterns among men and women in collegiate basketball and soccer: NCAA data and review of literature. Am J Sports Med 23(6), 694-701.
Bahr, R., & Krosshaug, T. (2005). Understanding injury mechanisms: A key component of preventing injuries in sports. Br J Sports Med 39, 324-329.
Collins, M. & Raleigh, S. (2009). Genetic risk factors for musculoskeletal soft tissue injuries. Med Sport Sci 54, 136-149.
Cannell, J., Horris, B., Sorenson, M., Taft, T., & Andersen, J. (2009). Athletic performance and vitamin D. Medicine and Science in Sport and Exercise 1102-1111.
Freckleton, G., Cook, J., & Pizzari, T. (2014). The predictive validity of a single leg bridge test for hamstring injuries in Australian Rules Football player. Br J Sports Med 48, 713-717.
Hullin, B., Gabbett, T., Blanch, P., Chapman, P., Bailey, D., & Orchard, J. (2014). Spikes in acute workload are associated with increased injury risk in elite cricket fast bowlers. Br J Sports Med 48, 708-712.
Kiesel, K., Plisky, P., & Voight, M. (2007). Can serious injury in professional football be predicted by a pre-season functional movement screen? North American Journal of Sports Physical Therapy 2(3), 147-158.
Lauersen, J., Bertelsen, P., & Andersen, L. (2014). The effectiveness of exercise interventions to prevent sports injuries: A systematic review and meta-analysis of randomised control trials. Br J Sports Med 48, 871-877.
Meeuwisse, W. (1994). Assessing causation in sport injury: A multifactorial model. Clinical Journal of Sport and Medicine 4, 166-170
September, A., Cook, J., Handley, G., Van der Merwe, L., Schwellnus, M., & Collins, M. (2009). Variants within the COL5A1 gene are associated with Achilles tendinopathy in two populations. Br J Sports Med 43, 357-365


