
Michael Tankovich, PT, DPT, ATC, L/AT, CSCS, Physical Therapist/Assistaint Athletic Trainer, Seattle Seahawks Football Club
One of the sharpest minds in sports medicine and recovery science is Michael Tankovich, a physical therapist with the Seattle Seahawks. World Class therapy can only be achieved when the therapists understand training and can compliment their approaches to a team environment. Cutting edge technologies such as Heart Rate Variability and GPS tracking is widely available, but it’s the application of methodologies and the organization of all approaches that make a program successful.
Carl’s Note: After bumping into one of my former athletes who worked with “Tank” I was so impressed that I had to do an interview. When we think about NFL therapy, we usually think triage style support and not individualized care. Many great people exist that work insane hours doing the right things, and finding them isn’t easy. I would like to thank Michael Tankovich for taking time from his break and responding to my questions with depth and expertise.
Dry Needling and Neuropeptide Responses
Freelap USA — The NFL is dealing with management of main and you are trained in Dry Needling, showing some interesting findings with the Autonomic Nervous System, surface EMG and thermography. Since the therapy is not something athletes can do on their own or be scaled easily, when do you think is the best option to add that modality?
Tankovich — I know dry needling is somewhat controversial, so first I will give a little background on how I view manual therapy of all types and where dry needling fits in our program. This quote by Boo Schexnayder sums up how I see the continuum of rehabilitation from injury:
The basic premise is that throughout the rehabilitation process, the tension levels applied to the injury site must progressively increase until they reach competition level intensity.
I would add that the nervous system must also deem ‘competition level intensity’ as non-threatening or non-painful. It really is that simple; however, the art of achieving that goal is where things become complicated. Many roads lead to Rome and every athlete will respond to treatment and rehab in their own way. Regardless of the type, manual therapy does not “fix people,” but it can lead to changes in movement, reduction of pain and faster return to activity.
With all that said, I have found dry needling (as I have learned it through the Kinetacore education programs) to be a very powerful input that leads to positive changes with many of the athletes that I work with. Due to time constraints, I mostly use it with injured athletes to address (SFMA based) movement dysfunction and for direct treatment of injured areas. In my experience, dry needling provides a quick and long lasting relief of tight areas as compared to other forms of manual therapy.
Carl’s Take — Boo’s thoughts on rehabilitation are very progressive and the continuum Michael Tankovich speaks of is one of the best concepts in rehabilitation and return to play. Many approaches simply look for handling pain and skip the progression of tension on tissues and create additional dysfunction and re-injury. The goal of smart return to play is not to return faster per se, but to return more complete and ready for sport. While tension is a continuum, most activities are more milestones in the return to play pipeline, such as progressing from fast tempo runs to sprinting.
Freelap USA — Recent advancements with electromedicine and tendons are growing in popularity in Spain and are already being used in Canada. Do you see a combination of electrotherapy and dry needling growing to something more sophisticated?
Tankovich — I think we will see an explosion of research on dry needling and the use of electrical stimulation over the next few years. While medical treatment with needles is not a new idea, research shows many novel approaches are being created. For example, recent research has shown that changes in electrical stimulation frequency can influence the release of different neuropeptides. Also, I have found that treating athletes in the position of provocation and or tightness has shown great outcomes, especially in cases of adverse mechanical neural tension. I also think some of the new research on accelerated healing of tendon and ligament injuries will prove valuable to the sports medicine field. As dry needling grows, evaluations will improve and we will see more specific and direct approaches to treatment.
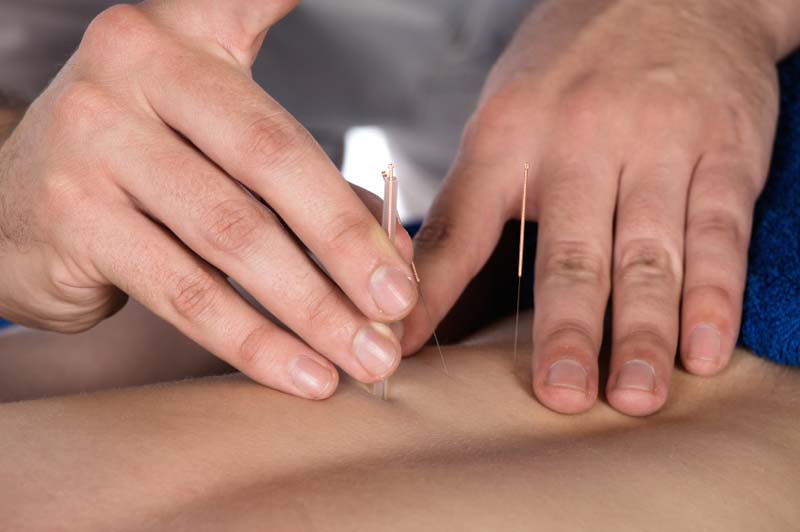
Figure 1: Dry Needling
Carl’s Take — Neuromodulation is nothing new, and the SetPoint company is implanting micoregulators straight to the vagus nerve to control inflammation. The implant used can be controlled by an iPad and has its own platform currently. MC10 was innovative using sensors that are applied to the skin, but now we are at the biopunk stage of sport that athletes will have implants in the near future. The inflammation cascade is very similar to controlling and managing wildfire, as nature needs inflammation to grow (adaptation) but uncontrolled levels can create a major problem long term with athletes. A team can see the true biochemical stress load on each athlete and manage pain and strain better by using stress hormones and biomarkers every month or so.
Comprehensive Screening and Evaluation
Freelap USA — Screening athletes with different movement tools is evolving and many teams are looking at reducing injuries by ensuring athletes can hit benchmarks such as scores in the FMS and other tools. How much buy in do athletes need to appreciate such scores so they care independent and take ownership with both recovery and corrective approaches such as remedial exercises?
Tankovich — Trying to predict injuries and intervene to prevent them is no small task. Despite all the screening tools, sports injuries continue to increase. One thing I have learned over the past few years is that you can’t rely on a single screening tool and expect perfect results. The FMS is a starting point to assess general movement abilities, but its simplicity is also its limitation. The FMS only measures an athlete’s ability to move in a slow static environment. It does not give you information on how an athlete is able to handle load and absorb and dissipate high velocity forces. We can gain a general sense of an athlete’s mobility from the screen as well as the motor control strategies they choose during the tests, but we must understand that motor control is context specific. It’s a stretch to assume athletes will choose the same motor control across varying tasks, especially as load and velocity increase. The FMS is a useful part of our screening process; however, it is important to understand the test’s limitations so you can fill in the gaps with other tests or measures. Part of this is being observant, noting how the athlete moves during the warm up, how they run and how they decelerate. These are all important things to be aware of. Movement screening is a daily process.
Freelap USA — What are your thoughts why some football athletes don’t connect with the knowledge of sport medicine and performance?
Tankovich — We are most concerned with the overall health and performance of our players. If an athlete does not respond well to the FMS we look into other ways to raise their general wellness. Some players respond better to using objective measures and tracking for both performance and lifestyle changes. You may not always change a player’s FMS score, but if they’re sleeping an extra hour every night and eating better, it’s still a win.
Carl’s Take — Compliance can be measured, and that ranges from attendance to the most sophisticated of sleep metrics incorporating biomarkers and player tracking. The FMS and other movement screens need to involve more data that is actionable, such as seeing if muscles are not active (SEMG), joints are mobile (motion capture and pressure mapping) and fatigue is not creating compensation (physiological monitoring).
The Lymphatic System and Recovery
Freelap USA — Aquatic exercise and Pneumatic Compression devices such as Normatec are part of the recovery system of many teams, but the key is applying it in an organized fashion. You have an internal system that is quite effective and have evolved each year in application of recovery. When you look at recovery without the use of HRV and go right into communicating with athletes, what lessons have you learned from face to face that are not replicated with technology?
Tankovich — Managing recovery for an entire football team is no easy task. Our approach has evolved and improved over the last few years. Obviously the best recovery program is a good training program (i.e. applying a load to the organism that stimulates the desired adaptation, then allow adaptation to occur, then stimulate again). Unfortunately, the training process is never that simple, especially when you are locked into a set competition calendar season. It is during these times that using recovery modalities become important to improve an athlete’s stress resistance.
The first step to improving recovery is to develop a culture of knowledge. We educate athletes so that they understand the benefits of doing extra recovery work. Part of this process is to provide easy-to-follow protocols that guide the athletes through their recovery program (pool recovery, contrast pool programs, sauna recovery, Epsom salt baths, etc.) We invest time and take the athletes through their program to make sure they understand, which is a huge benefit to us in the long run.
The next step is to add variety to recovery programs. Many players have “go-to” recovery modalities that they use over and over. For example, a number of players like to use the cold tub every day, sometimes multiple times a day. This repetition can cause the player to adapt to the cold tub and it will begin to lose effectiveness. For these players, we create periodized recovery programs to add variety to their current programs.
We are also currently working toward adding specificity to our recovery modalities based on Omegawave testing and subjective questionnaires, but for now we just want the athletes doing a variety of recovery. I think active recovery (pool, bike, mobility work) has advantages that passive recovery lacks, but when athletes are tired and beat up following a practice, they may not want to get in the pool and move around. Those are the times to apply passive recovery such as NormaTec or contrast pool programs. On off-days active recovery, especially the pool, is great for players who have general soreness and/or tightness. I can’t think of a case where an athlete finished a pool recovery program and didn’t feel better.
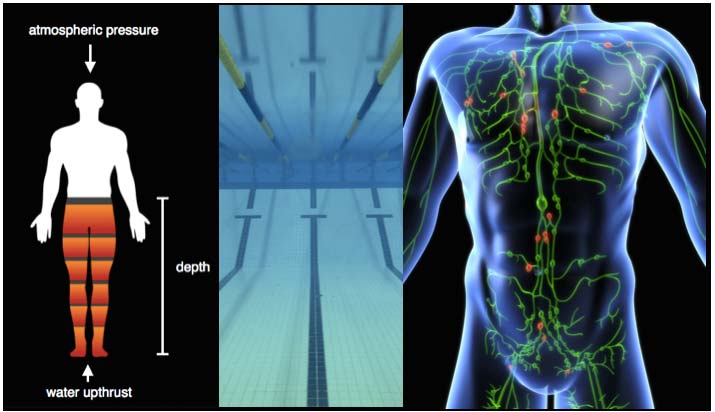
Figure 2: Hydrotherapy and Pneumatic Compression
Carl’s Take — Hydrotherapy or pneumatic compression can accelerate recovery at the phase level, meaning over weeks. Cytokine overload will impair total testosterone and may create complications with the SHBG of athletes who are doing too much. By adding regular sessions of pool or pneumatic compression, athletes will have a measurable difference in inflammation in my experience doing blood panels. Some land based circuits can help take advantage of the “second heart” of the leg pump, but the lymphatic system can move more free proteins with aggressive aquatic work or compression therapy.
The Challenge of Large Rosters in the NFL
Freelap USA — Some teams in Europe have an excellent therapist to athlete ratio, but in American Football the ratio is worse than any sport because the roster size. Many European consultants suggest various solutions that can’t be scaled with the NFL since soccer is smaller and has more staffing. Besides student support (interns and massage schools) what do you think about effective ways of using time?
Tankovich — This is a great question, and one that is a significant issue in American sports. We host a European soccer club at our facility each summer, and it’s amazing to see the size of the staff they have. The more hands you have the higher the potential quality of care. With that said, no matter the size of your staff there is no point in making excuses. I get to work with an incredible staff of athletic trainers and physicians, and I learn time and time again how important it is to master the basics and pay attention to details. Our vision is to provide a level of care that our athletes cannot receive anywhere else. We have the budget to purchase a variety of technology and continuing education that would be difficult for private facilities to match. The difficult part is putting in the hours to provide individual care to all of our athletes. It makes for busy days and long hours, but our time and energy is a direct investment in our player’s health.
Freelap USA — Doing a TMG reading takes 20 minutes on an entire body and that could be all one has with a player, anything clever you have seen to be more efficient with time in general?
Tankovich — In general, our approach is no athlete left behind. We try to provide the best care possible to each and every player. This means quick assessments that can be completed fast and reassessed daily. For this, we use the SFMA and/or osteopathic hip assessments to guide daily interventions. It’s not perfect; it’s evolving, but it’s better than nothing. I have also used specific movement baselines to guide daily loading in late stage rehabs. If an athlete is returning from a hamstring strain, I will use the active straight leg raise test before and after running workouts. If they tolerate the load and intensity well, we expect to see similar pre-post test results. If they have a decrease in active range, this may signal that the nervous system is guarding and the loading may have been more than they were ready for. I want to see a return to baseline or better before repeating the workout.
Carl’s Take — The hardest data to collect is medical findings and I will always refer to Equine Sport to get the most creative ways to capture and analyze data. The reason is, horses are experiencing the same pattern of injuries as human athletes with more and more breakdown. The future is available now, meaning visual and conversations can be recorded, filtered, calculated, and presented graphically to allow all parties to understand the problem easier and faster. Such technologies will be shared in an interview with Jose Fernandez, an excellent resource in sport health and performance.
Peaking Starts in the Pre-Season
Freelap USA — Congratulations on the Super Bowl win and it seems that you guys peaked when it counted. With every team having access to the same tools and information, what do you think the NFL can improve on with reducing injuries?
Tankovich — Football is a sport driven by tradition; it is difficult to make changes or progress quickly. We have seen small changes in the rules of the game over the years to help combat the risk of injury, but I believe changes need to happen in player preparation as well before injury can be eliminated. One issue is a lack of organized training time without competing coaching demands. Currently, strength coaches get a total of two weeks a year to prepare players for the rigors of practice without competing for adaptive reserves from practice. Despite all the injury risk assessments, we can’t forget the greatest risk of injury is previous injury, followed by a sharp increase in training load. A longer training period would allow strength coaches to gradually build up to practice intensity and volume over time, versus having a large spike.
Pre-season training camp is typically the greatest training load the players will have all year. Prior to this camp, the players are on a five-week break. Many players do a good job of training during this time, others not so much. It is difficult to simulate the training intensity that happens with coaches. I think it will be very difficult to eliminate injuries until the schedule changes or the league begins to understand the importance of graded exposure.
Carl’s Take — The NFL and NFLPA have to agree that controlled training during pre-season requires more time and more gradual introduction to heavier and faster loads. Ironically, many teams are trying to do more with less time, compounding the problem and making the injury rates worse. Athletes are not likely to stay with the team during the break and this can be either a major problem or a benefit depending on who the athlete works with. With large rosters and small therapy teams, it’s essential that athletes leverage the break during the summer and invest into their bodies and not just take time off. Some private facilities are excellent resources and some are slaughterhouses, so agents, management, athletes, and staff will need to collaborate more or the NFL will see another rise in non-contact injuries.
Freelap USA — Besides administration and technology, what areas do you think teams should work on with team coaches and sport science and sports medicine?
Tankovich — I am lucky to be part of a progressive organization that is interested in advancing our philosophy on player health and performance. We are constantly adding new ways to strive for continued success in injury prevention. Most recently, with the addition of data collection and management, we are beginning to recognize injury trends and patterns. This evidence will lead to improvements in athlete screening, injury management and practice/training load regulation to reduce injury and improve performance.
Carl’s Take — I have mentioned this over and over again, but the next step is moving from athlete tracking such as GPS and Prozone, to areas of risk such as individual points, down to individual bones in the foot to site-specific locations of the hamstring. As we understand gross loading of the body, we will be able to move to very local areas of joints, tendons, and muscles. We are at the moment of time that we can drill down to the fifth metatarsal joint with risk and we need to evolve beyond just gross loading descriptions.
Please share this article so others may benefit.
[mashshare]

